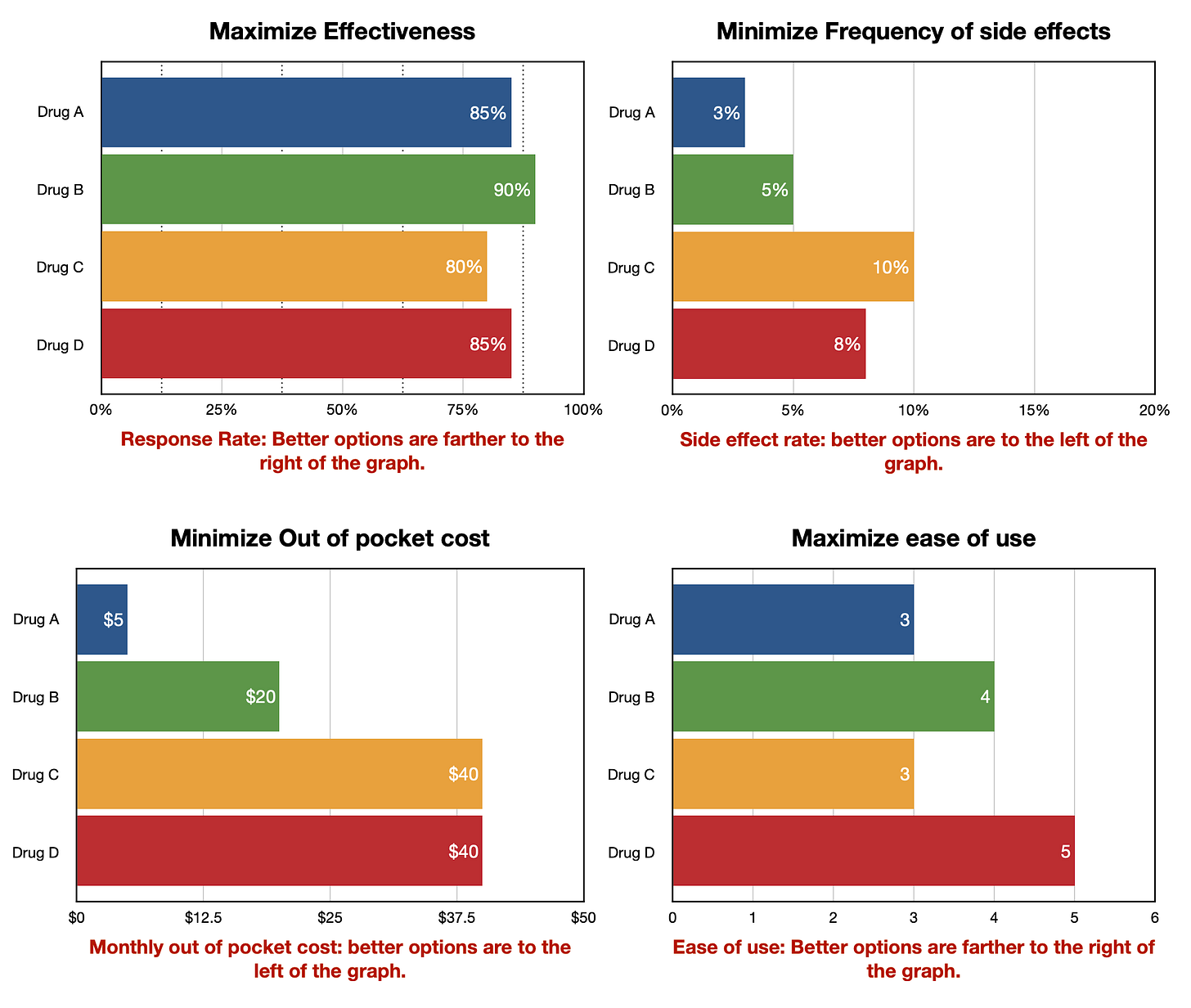
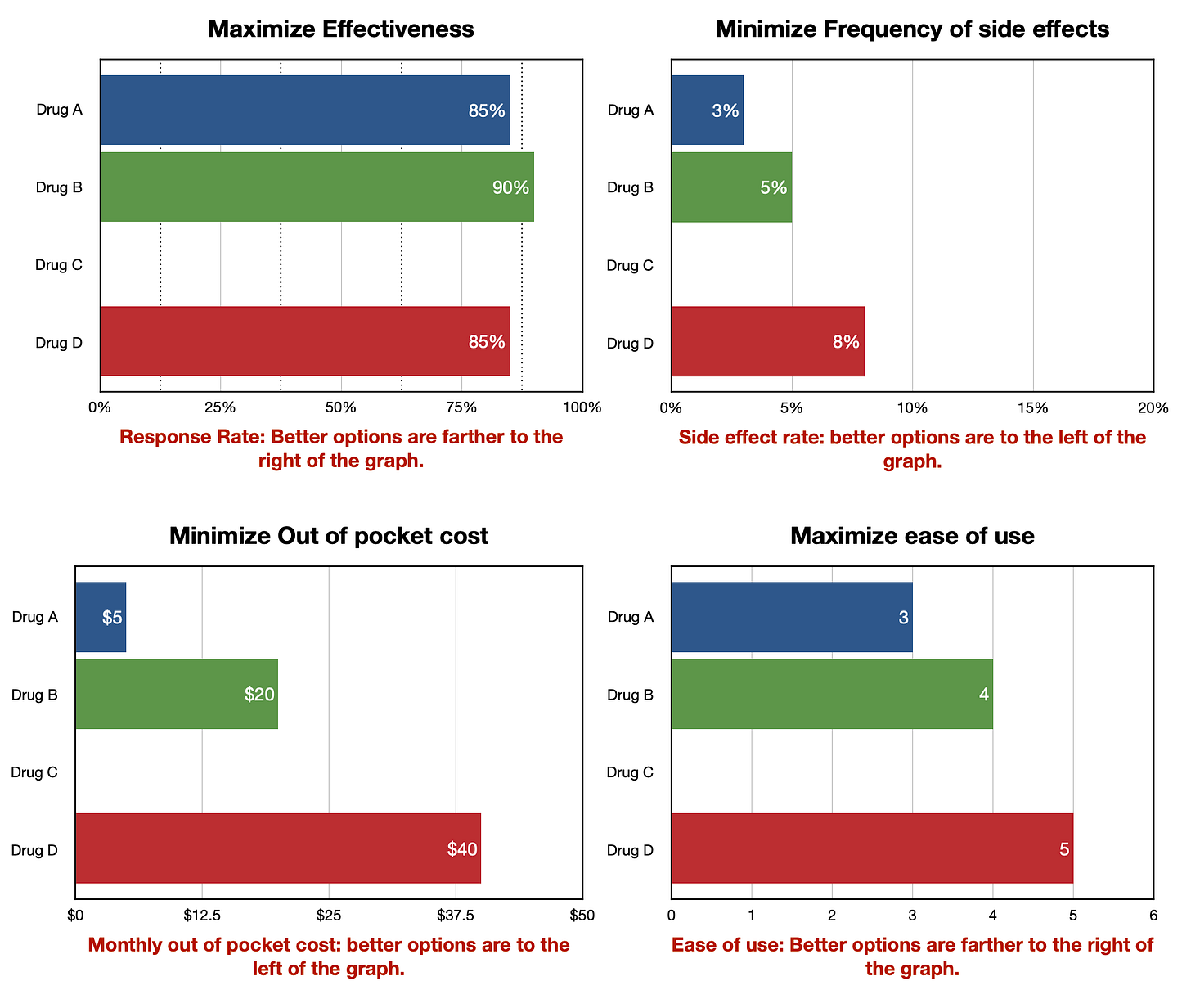
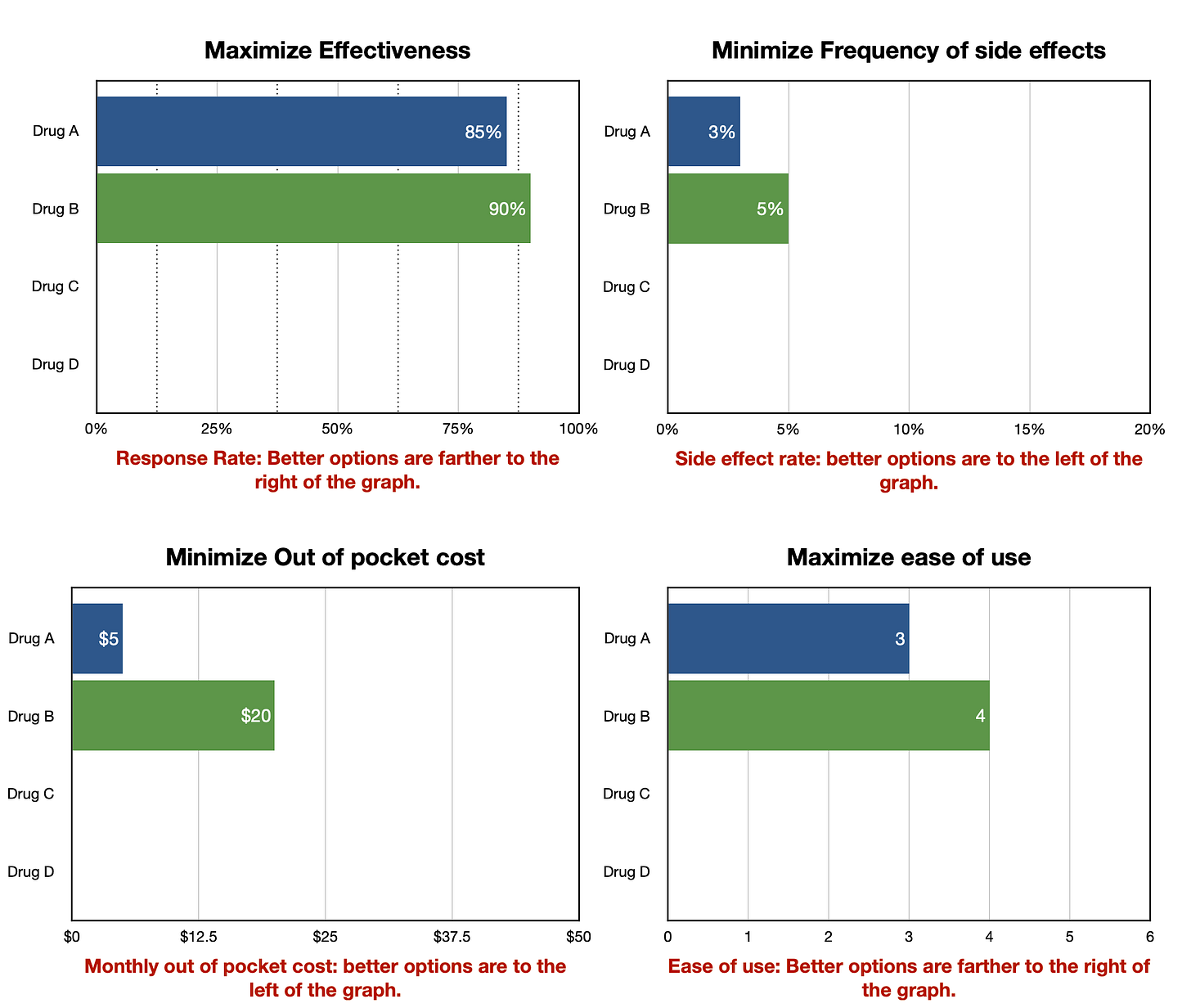
Our motto could be the following: focus on identifying and solving problems with decision-making rather than moving the needle on decision-quality measures. [1]
In recent Musings, I have been exploring the concept of decision quality and ways to improve the quality of routine clinical decisions.
In the November 18, 2022 Musing, I suggested that finding a way to help clinicians and patients become better decision makers could speed implementation of shared decision making in clinical practice and improve the overall quality of medical decision making. In more recent Musings, I proposed using the Decision Quality Chain, developed by the Strategic Decisions Group, both to guide the clinical decision making process in real time and to measure the aggregate quality of clinical decisions.
I was, therefore, excited to find a newly published article by Peter Schwartz and Greg Sachs, titled Rethinking Decision Quality: Measures, Meaning, and Bioethics, published in the December 2022 Hastings Center Report. [1] Drs. Schwartz and Sachs are both Professors of Medicine at the Indiana University School of Medicine. In it, they analyze the concept of decision quality based on how it has been conceived and measured in the medical literature.
Schwartz and Sachs group existing decision quality metrics into three categories: Subjective measures that ask patients to reflect on a decision, Observational measures that evaluate decision quality by reviewing recorded conversations between patients and providers, and Informed-Concordance measures that objectively measure how well-informed a patient is about a decision and track whether they receive the option that best matches their preferences and values. They then discuss the advantages and disadvantages of each. Consistent with publication in a Bioethics journal, both the analysis and related discussion are focused on decision quality in terms of the bioethical goals of increasing patient autonomy and involvement in shared decision making.
The most well-known subjective measure is the Decisional Conflict Scale. [2,3] Although widely used, Schwartz and Sachs point out the shortcomings of relying on a subjective measure of how well informed a patient is and the fact that being more completely informed about a decision can decrease the measured quality of the decision by adversely affecting scores on the uncertainty and values clarification sub-scales. Measures on another commonly used subjective scale, the Decision Regret Scale [4] – which measures regret months after a decision is made – confounds measurement of the quality of decision by knowledge of the outcome. This is because, when decisions are made when the outcomes are uncertain, as the majority of healthcare decisions are, good decisions can result in bad outcomes and vice versa.
Examples of objective measures include the Informed Decision Making Scale and the OPTION scale. [5-7] While they are not subject to the limitations of the subjective measures, they are logistically difficult and run into concerns for patient privacy. Schwartz and Sachs also point out that they may not always accurately reflect a superior decision making process, particularly in the setting of an ongoing provider-patient relationship that involves multiple interactions in addition to the one being evaluated.
Problems with the Informed-Concordance measures such as the Multidimensional Measure of Informed Consent [8] include difficulties defining what knowledge is essential for the patient to know about the decision being considered and determining what the optimal choice is for any given patient.
Based on their analysis, Schwartz and Sachs reach three conclusions:
1. While each type of measure captures something important, none of them captures all the important components of decision quality.
2. Decision quality is complicated and cannot be adequately captured in a precise quantity. Instead of trying to measure quality using a precise quantitative value, it is more appropriate to describe it using general terms such as good, satisfactory, or poor.
3. Efforts to improve clinical decisions should “… focus on identifying and addressing cases of poor or problematic decision-making, rather than on improving the mean score on a measure or combination of measures.”
Musings
This is a terrific contribution and everyone interested in shared decision making and the overall quality of clinical care should read the full article. However, it has a couple of limitations that are worth keeping in mind:
1. The analysis was limited to how decision quality has been conceived and characterized in the medical decision making literature. Healthcare is not the only field where good decision making is important and, as pointed out in prior Musings, there is a wealth of information about how to improve decision making in applied settings available that could easily be imported from other fields to address current problems with medical decision making. For example, the Decision Quality Chain is a well-developed crystallization of the elements that define a good decision that can be readily understood and used to guide and evaluate the quality of a decision process. (See the December 2, 2022 and January 13, 2023 Musings for details.) For this reason, I think the authors’ second conclusion, while correct given how decision quality has been conceived in medical settings to date, should not be generalized beyond the limits of the literature reviewed.
2. The authors don’t comment on a major shortcoming of all current measures: they involve an extra step to obtain the quality measurement, making them primarily research tools rather than methods to improve the ongoing quality of decisions in practice settings. To be truly effective, measures to improve clinical decision making , particularly those involving important bioethical goals such as involving patients in decisions about their healthcare, need to be effectively integrated into routine practice. Using a measure of decision quality, such as the Decision Quality Chain, that can be used to both guide on an ongoing decision making process and generate information useful in evaluating the aggregate quality of decisions makes sense to me.
Despite these limitations, I agree with the primary message of the article: it is time to to improve the quality of clinical decision making by instituting programs to diagnose and cure problematic clinical decision making practices at all levels of the healthcare system.
References
1. Schwartz PH, Sachs GA. Rethinking Decision Quality: Measures, Meaning, and Bioethics. Hastings Center Report. 2022;52(6):13–22.
2. A. M. O’Connor, “Validation of a Decisional Conflict Scale,” Medical Decision Making 15, no. 1 (1995): 25-30.
3. M. M. Garvelink et al., “Decisional Conflict Scale Use over 20 Years: The Anniversary Review,” Medical Decision Making 39, no. 4 (2019): 301-14.
4. J. C. Brehaut et al., “Validation of a Decision Regret Scale,” Medical Decision Making 23, no. 4 (2003): 281-92.
5. Braddock CH, Fihn DS, Levinson W, Jonsen AR, Pearlman RA. How doctors and patients discuss routine clinical decisions—informed decision making in the outpatient setting. J Gen Intern Med 1997;12:339–45.
6. Braddock CH, Edwards KA, Hasenberg NM, Laidley TL, Levinson W. Informed decision making in outpatient practice—time to get back to basics. J Am Med Assoc 1999;282:2313–20.
7. Elwyn G, Edwards A, Wensing M, Hood K, Atwell C, Grol R. Shared decision making: developing the OPTION scale for measuring patient involvement. BMJ Quality & Safety. 2003 Apr 1;12(2):93-9.
8. Michie S, Dormandy E, Marteau TM. The multi-dimensional measure of informed choice: a validation study. Patient education and counseling. 2002 Sep 1;48(1):87-91.